Hospital Calls Police to Stop Texas Sheriff Deputy Getting Ivermectin: 'The Medicine Will Kill Him’ (Part 3)
Exclusive first interview with Erin Jones who is trying to save her husband Jason Jones from dying of COVID
EXCLUSIVE SERIES: This is part three in an exclusive 9-part series on a dying Texas Sheriff Deputy suing for the right to try Ivermectin for COVID.
To catch up, read part 2 here: Hospital's New Hurdle to Stop Texas Doctor from Giving Ivermectin to Dying Sheriff Deputy (Part 2)
Erin Jones is desperately trying to save her 48-year-old husband from dying of COVID.
Jason Jones, a Tarrant County Sheriff’s Deputy, has been on a ventilator since Oct. 7. Erin asked Jason’s doctor at Texas Health Huguley Hospital for multiple treatments she’s researched, but he refused.
To get caught up on the Jones case, read my first story in which I kept their names private. Erin decided to let me make their family’s story public in the hopes she can get more public support to treat her husband.
Erin hired a lawyer, found a new doctor and got a court order for other treatments, including Ivermectin. But when she and a nurse got to the ICU door to administer the first dose on Wednesday, the hospital called the police to stop her.
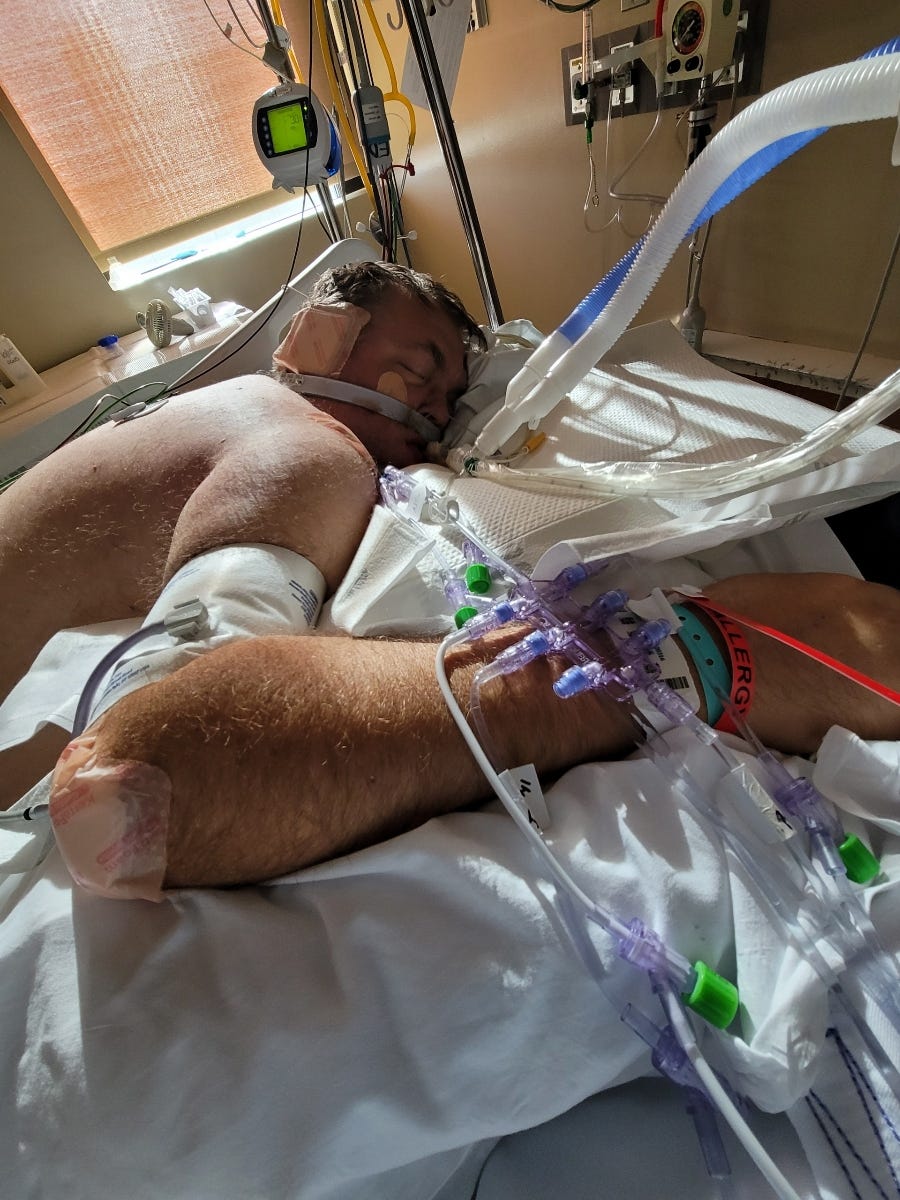
On Friday, the hospital wrapped a towel around the feeding tube to block Erin from administering the Ivermectin herself. She took the photo of it below.
The hospital calls the cops
Erin checked in at the hospital desk on Wednesday evening. She told the guard that she had a court order which would allow the nurse with her to be a second visitor to Jason’s room.
When she got to the ICU, she called on the security phone outside to have the doors opened, as she does every day. Erin told me that the head of the ICU, a man named Jason Cain, “showed up with hospital security and wouldn’t let us in.” The security guard told her that he was calling the police.
Erin said she welcomed the police because she had a signed court order -- which she showed him in hard copy. (Read the court order at the end of this story.)
Erin and the nurse also had the prescription that Dr. Mary Talley Bowden had written for Jason weeks ago. “Dr. Bowden wrote the prescription for Ivermectin to see if it will help,” she told me. “I’ve heard -- even now -- it could be able to help.”
By the time the police arrived, it was a scene outside the ICU. Three hospital administrators came to fight. One of them told the police officer that Dr. Bowden’s nurse had to be stopped because of the Ivermectin pills.
“‘The medicine will kill him.’ That’s what they said to the police,” Erin said. I checked with a police source who confirmed that the hospital administrator said the ivermectin would kill the sheriff's deputy.
Erin said she told the police and the hospital, “If I wanted to kill him, I would have done it some other way- I wouldn't have gone through this court process.”
Dr. Bowden told me, ”Before I started prescribing it, I looked at the original study on ivermectin presented to the FDA and saw no safety concerns. I then tried to find data on lethal overdose from ivermectin and found no published studies.”
The hospital staff showed the police another court document and said it was a stay by the appeals court. Erin said she didn’t know about this new document, but it did not have a judge’s signature on it.
“They wouldn’t show me anything — other than that 510-page thing— just scrolling and scrolling,” she said. “Beth, my attorney, said that is not the order that is the proposed order.”
Lawyer Beth Parlato is representing the Jones family. “We cannot do anything until it gets verified if there is a stay order. The appellate court was closed today for Veterans Day, so we can’t verify. We tried.”
Trying to get Ivermectin Early
On Sept. 20, Erin said Jason started “not feeling great” and the next day started running a fever. A couple of days later, they were running errands and decided to get something to eat. “I got him some potato salad, and he couldn’t taste it. And so he went to a lab and got tested, and it came back positive,'' Erin recalled.
She said a few days after the test, Jason started having breathing problems.
“We always go to Total Care. It’s not urgent, but they have doctors. And it’s just open better hours for his career,” she explained. She said the Total Care doctor prescribed him an antibiotic and steroid.
“We asked her for Ivermectin, and she said she wouldn’t prescribe it,” Erin said. “I tried looking online for Ivermectin and called doctors to try to get some prescribed, but I just didn't have the resources back then to get it.”
The next day, Jason had chest X-rays, which confirmed that he had pneumonia. The doctors said the steroids he had already taken “should be good.” But by that night, he was worse.
“He walked to the kitchen and came back to our room, and our daughter and I saw he was changing colors.” A relative who is a nurse told them he needs oxygen. “I said we knew the hospital was the last place we need to go.” But they went anyway to a Texas Health Hospital near where they live.
She said the hospital wanted to give him Remdesivir, but Jason refused. “He was worried about the kidney shutting down and liver failure. So he didn't want it.” She said they were concerned because they know another deputy at his department who passed away from COVID.
The hospital didn’t allow visitors for COVID patients. Jason didn’t want to stay. “He got into an argument with a doctor in the afternoon, Erin recalled. “He said, ‘Come pick me up. I’m done with them.’”
Erin took him back to Total Care when his oxygen level fell into the 50s. “The doctor said, ‘I have to call an ambulance.’” They told her Texas Health Huguley is right down the road and allows one visitor, so that's why they chose to go there on Sept. 28.
Her husband ‘went dark’
A week after he was in the hospital, Jason told Erin they needed to talk seriously.
“He went dark on me that day,” she said. “He talked about his career, talked about distributing things with our kids. I told him to stop it. But he said, ‘Just let me tell you these things.”
Erin said her husband told her, “They're going to kill me.”
I asked her if those were his actual words. She said yes. “He told me to hire an attorney because they are going to kill him. He felt that. He thought if he went on the ventilator he knew the odds weren’t great.”
The next morning, Oct. 7, Erin got an early morning call from the hospital. “They said, ‘We are intubating him. We’re putting him on a ventilator. You need to get up here,” she recalled. Erin raced to the hospital.
Everything moved fast around Erin in her husband’s crowded room. “I’m by myself, and he just grabbed my hand and told me he loved me and told me to give one of his guitars to his best buddy,” she recalled with emotion. “And that was the last time I heard his voice — through a BPAP machine.”
She added, “That was five weeks ago today.”
Hospital doctors blame COVID patients
Erin said Dr. Jason Andrew Seiden was Jason’s doctor until two days ago. “I don't know what happened. After the last court order was filed Monday, I went to his room and the nurse said Dr. Seiden is no longer on his case.” She did not like him anyway.
“Dr. Seiden told me, ‘It’s just a shame -- all you unvaccinated-- you get sick and come running to the professionals for help.”
Erin said she wishes she had her wits about her at the moment to respond.
“I would have said, ‘Doctor, just as if you were in a situation you would have called the police, my husband would have shown up and laid his life down for you and your family — that’s what you do if you’re a professional,’ Erin said to me, with anger in her voice for the first time.
She added, “Isn't that what everyone did before COVID? Get sick and go to the doctor?”
Read my story about Dr. Mary Talley Bowden, Jason Jones’s current doctor who only takes new patients who are unvaccinated here.
Erin said she is upset that Dr. Seiden changed what he said to her when they went to court.
“When he got intubated, Dr. Seiden said, ‘75 percent don't make it, so you need to cling to the 25 percent,’” Erin said. “But then we go into the hearing and he says now they are giving him a 10 to 15 percent chance of survival now. They were telling me things I didn't know. They told me he got COVID because he’s unvaccinated and he’s morbidly obese and now he has sleep apnea - but he’s never snored or stopped breathing in his sleep, so how would we know?”
Erin concedes that Jason was “not healthy” but that’s part of being in law enforcement.
“So stress, yes, his job is super stressful in these times. We know he wasn’t in top shape, I get it, but he’s not on any daily medications.” Erin said Jason was about 5’10” and weighed 240 lb.
She got frustrated by not having time to talk to the hospital doctors about alternative treatments to try. (Texas is a “right to try'' state which is noted on the court order, at the bottom of this email.)
“I was pretty much at my wit’s end, and that’s when I found out that everything goes through Dr. Seiden. He wasn’t willing to do anything that is not approved for COVID. He follows CDC, all these things, and that is just what he does.”
She asked for melatonin because he would take at home to sleep. “I think he got one dose and had a collapsed lung. He’s ended up with 5 chest tubes so far,” Erin said.
A Law Enforcement Family
The Joneses have been married for 23 years. They have six children. Their oldest daughter is a niece who they adopted when she was 10 years old. The other five range from 12 to 19 years old. Erin has been a stay-at-home mom since they took custody of their niece. Jason is the sole provider.
Erin said the other sheriff deputies tell her that they feel helpless. “They can't show up to the hospital in uniform. I understand. I’m not asking anyone to do anything to jeopardize their jobs, and that is why I went the legal way, she said.
Jason Jones’s favorite holiday was Halloween because he liked to do family themes. I told Erin that my favorite photo of their Halloween theme was the one below.
“We had such a good time with Kiss that year,” she texted back. “We did music videos in our living room and even got my dad to wear leather pants and my mom a choker necklace!!”
Erin was at her husband’s ICU bedside when I called her. She asked me to hold on while she got her things. “I don’t like to talk on the phone in his room,” she said when she was in the hallway.
She headed to her car— through the atrium of the hospital.
“You know what burns me?” asked Erin. “It’s extremely hard to walk through this atrium because they have pictures of Christ touching people and healing them.”
Keep reading…. click below to read part 4 in my exclusive series on Deputy Jones:
Note To my paid subscribers — Please keep this between us, but I am close to being deplatformed on Facebook for writing about Ivermectin. I’ve been able to fight back and regain my account out of the public eye, so far. Frankly, I would rather stay silent about their censorship than lose a platform to reach a wider audience on this important health issue.
However, I want you to be careful posting this story on your own Facebook pages so you’re not caught up in this. Facebook is my biggest source of new subscribers and traffic, but I can’t stop reporting out of fear of their power.
I have been thinking a lot lately that perhaps the purpose of this substack newsletter might be to give a voice to the underdogs in major political fights, rather than a place to write about policy and political facts. I think about all the people in Afghanistan who need their voices heard, people losing jobs over vaccine mandates and those who want to exercise Second Amendment rights who cannot. Would you be interested in reading more personal accounts like this story about Erin and Jason Jones? Let me know in the comments (which are only for paid subscribers.)
Thank you for sticking by me and supporting me through all these difficult topics I take on when other reporters refuse.
LINKS TO SOURCES:
Fundraiser for Jason Jones and Family on Give Send Go
Texas Health Huguley Hospital website
Dr. Bowden’s practice Breathe MD is here, Linkedin, Twitter
Dr. Jason A. Seiden, MD, FCCP practice NTX Lung and Sleep
Front Line COVID-19 Critical Care Alliance (FLCCC) website
Government Information on Ivermectin as a treatment for COVID-19: National Institutes of Health (NIH), World Health Organization (WHO), FDA









I saw the stories below the recent one about Baldwin and went down this rabbit hole…
It is insane, I N S A N E that this ever happened. I’d like to hear what those doctors think now. Or the people who stood at the doors of Walmart and HEB Grocery telling people to put on masks.
Reading these stories today is like a fictional work. One question that hasn’t been answered that they don’t want to answer: How the hell did this happen in The United States of America?
Please keep up your wonderful work Emily!